
Photo by Nigel Baker Photography/Shutterstock
If you’ve been around horses a while, you’ve probably seen the following: a horse (that isn’t a stallion) with a really thick crest and fat pads along the withers, at the base of the tail, and virtually anywhere along the trunk. The horse may also have fat deposits in the fossae above the eyes. While we could think a horse like that is just obese, he could also be suffering from a serious condition that needs medical management.
Approximately 10 percent of horses in the United States have been diagnosed with insulin resistance. Insulin resistance is a type of equine metabolic irregularity that falls under the umbrella of equine metabolic syndrome (EMS). In addition, another 10 percent of horses who have Cushing’s disease, or pituitary pars intermedia dysfunction (PPID), are also insulin resistant.
What does it mean if your horse is part of these statistics?
What is Insulin Resistance?
The term insulin resistance has only become well recognized in the last 15 years. With a horse like the one described above, there are internal forces at work that cause these clinical signs.
“Insulin resistance is a state where insulin-dependent cells of skeletal muscle, fat, and liver don’t respond normally to insulin, requiring higher levels of insulin to get them to take up glucose from the blood,” says Eleanor Kellon, VMD. Kellon is currently the staff veterinary specialist of Uckele Health and Nutrition, based in Blissfield, Mich. She is also the owner of the consulting business Equine Nutritional Solutions and the owner and volunteer veterinary advisor for the Equine Cushings and Insulin Resistance (ECIR) Group, Inc., which provides the latest research, diagnosis, and treatment information for horses with these conditions.

Skeletal muscle consumes glucose, therefore a regular exercise program is extremely important for managing IR. Photo by Horsemen/Shutterstock
Although there are some situations where a horse may only be insulin resistant for a short time, generally the condition has a genetic component and is one that the horse will face long-term. While Thoroughbreds, Standardbreds, warmbloods, Quarter Horses, and full-sized draft breeds are generally at the most risk for IR if they are diagnosed with PPID, the Morgan, Arabian, Andalusian and other Spanish breeds, Miniature Horses, gaited breeds, Fjords, Icelandics, and most ponies are automatically considered high risk.

Arabians, Morgans, Spanish and gaited breeds, Fjords, Icelandics and most ponies are considered high risk for insulin resistance. Photo by Alexia Khruscheva/Shutterstock
“Things like some drugs and serious infections may cause temporary insulin resistance, but otherwise, the cause is genetic,” Kellon says. “Because it is genetic, the tendency to have high insulin will always be there, but most horses can be well controlled by diet and exercise.”
Outside of the genetic component, or potentially a diagnosis of PPID, mares in the last half of pregnancy can also develop the condition.
Getting Older
Close monitoring of your horse becomes even more important at certain stages of his life.
“Problems typically start to develop after horses reach physical maturity, when their calorie requirements drop,” Kellon says. “It also develops quickly in susceptible horses if they have a large drop in their level of exercise.”
Cases related to PPID will develop metabolic signs in their teens or 20s.
“Developing laminitis for the first time later in life is often the first indication of PPID,” she adds.
Reaching a Definite Diagnosis
If you suspect that your horse is insulin resistant, consulting with your veterinarian is the best place to start for a definitive diagnosis and treatment options.
“I always advise people to test,” Kellon says. “Looks alone are not enough for a diagnosis, and it’s important to know how high insulin is and if glucose is normal. If a horse doesn’t have a problem, it can save a lot of worry and stress about feeding. Insulin can be tested at baseline, fasting, or non-fasting (hay or pasture only), and there are challenge tests where the horse is fed grain, dextrose on a chopped hay base, or Karo syrup.”
As for the timing of testing, the jury is still out on the best season and time of day. However, there is anecdotal evidence that insulin levels in the bloodstream are very erratic in cold weather.
“If you have an issue, I would still test then and treat, but realize that the insulin may level out a bit in warmer weather,” Kellon says. “The research is divided on whether or not there is a seasonal rise in insulin in autumn. In terms of the [best] time of day to test, if you make sure the horse has constant access to hay or pasture from the night before through the day of testing, anytime is OK. Do not exercise or ship the horse before testing.”
Once a diagnosis has been reached, important comorbidities to consider include laminitis and obesity.
“It has been estimated that around 90 percent of all laminitis cases are caused by elevated insulin,” says Kellon. “Obesity is a common comorbidity, but not always present.”
Signs of Laminitis
If you own a horse that is suspected to be insulin resistant, you should become thoroughly familiar with the subtle warning signs of smoldering laminitis.
“High insulin causes damage to the [hoof] laminae even in horses that have never had a full-blown laminitis episode,” says Eleanor Kellon, VMD, staff veterinary specialist at Uckele Health and Nutrition, owner of Equine Nutritional Solutions, and owner and veterinary advisor for the Equine Cushings and Insulin Resistance (ECIR) Group, Inc. “This is often hard to spot because both feet are equally affected.”
Signs include:
◆ Stiffness at the walk with loss of normal side-to-side sway
◆ Stiff head carriage
◆ The head held either higher or lower than normal when moving
◆ Reluctance to make sharp turns
◆ Hesitation to move off from a standstill
◆ A preference toward soft ground
◆ A slower, shortened stride on hard footing
If you notice any of these signs, talk to your vet about testing and treatment for insulin resistance. A good program should help clear up these signs of low-grade laminitis.
Treatment Options
Successful treatment for insulin resistance lies in a foundation of diet and exercise.
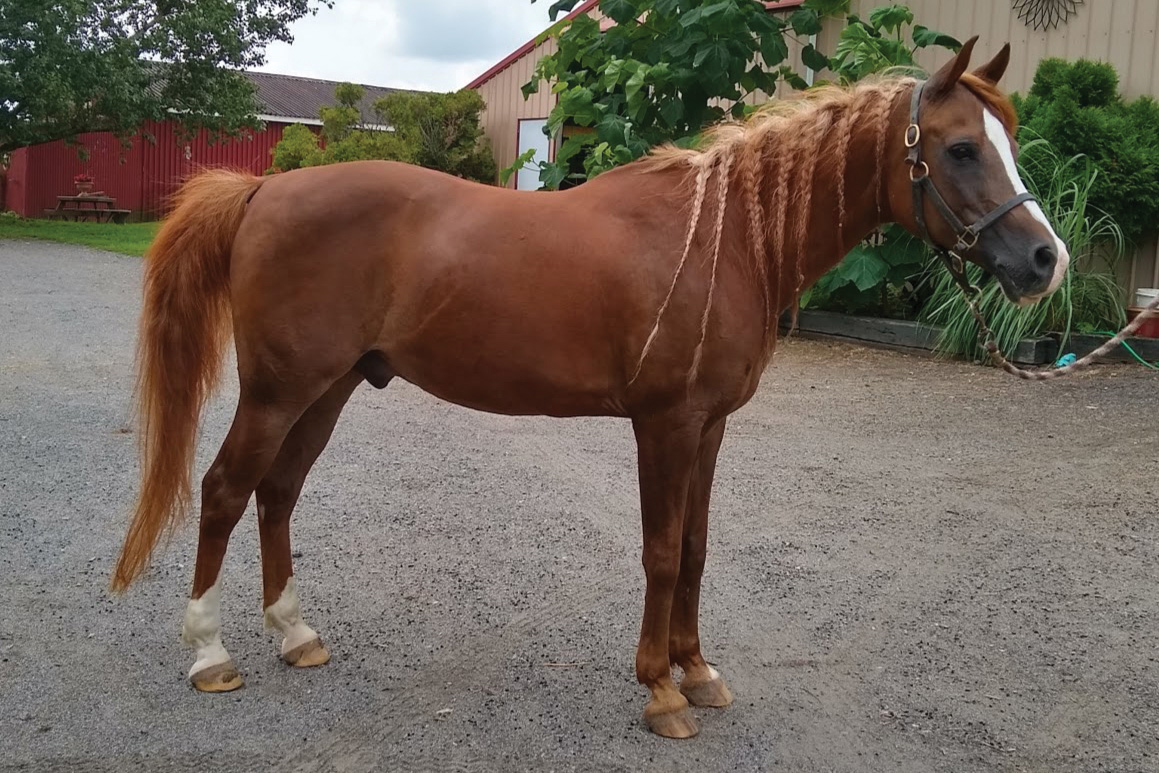
The author’s half-Arabian mare grass foundered at age 5 and has been treated for insulin resistance in the 15 years since. With the help of living on a dry lot and a restricted diet, she was able to have a successful show career, including some limited jumping. Now she is a semi-retired trail horse. Photo by Hope Ellis-Ashburn
Kellon recommends feeding insulin resistant horses grass hay with a combined sugar (ethanol-soluble carbohydrates, aka ESC) plus starch content of 10 percent or less, fed at 1.5 percent of current body weight or 2 percent of ideal body weight, whichever is larger.
“Carriers for minerals, such as feedstuffs to balance the diet, should be less than 10 percent sugar plus starch,” Kellon adds.
She recommends analyzing your horse’s hay for mineral content so supplementation can be customized to the hay. Some considerations should be kept in mind, like a calcium to magnesium ratio no higher than 2:1 and iron to copper to zinc ratio of 4:1:3.
Soaked, well-rinsed beet pulp is an ideal feed for IR horses. The Equine Cushing’s and Insulin Resistance Group, Inc., maintains a list of other safe feeds.
Exercise is also very important. Turnout, while better than a stall, does not equate to exercise.
There are medications available for horses whose insulin resistance can’t be controlled with diet and exercise alone. Usually, these horses are plagued with chronic laminitis.
“Metformin has the longest history of use but doesn’t work for some and may lose effectiveness over time,” Kellon says. “A group of drugs called SGLT2 inhibitors is being investigated and showing promise. Other than mineral balancing and some supplements to help with laminitis, there are no effective supplements for metabolic syndrome.”
Pasture grazing is risky for a horse with insulin resistance, both because sugar is higher in fresh grass and because levels change significantly from day to day.
“Spring and periods of rapid regrowth are particularly dangerous, but nothing is guaranteed safe,” Kellon explains.

An IR horse should be kept off grass until his condition is well-controlled and he is back to a significant exercise level. After that, the horse should only be allowed to graze for 30 to 60 minutes, and only immediately after exercise. Photo by Anjajuli/Shutterstock
She suggests horse owners avoid allowing an IR horse to graze until the horse’s condition is well-controlled and he is back to a significant exercise level. After that, the horse should only be allowed to graze for 30 to 60 minutes, and only immediately after exercise. Skeletal muscle is the major consumer of glucose in the horse’s body.
“Exercise results in glucose uptake by pathways that do not require insulin, thus relieving the pancreas and insulin of much of their work,” Kellon says. “The effect is strongest for an hour or so after exercise, but still present 24 hours after exercise. As the horse becomes fit, the improved insulin levels and reduced insulin resistance will last for as long as a month after regular exercise is stopped. It’s common to hear of IR-prone horses, like Arabians, that had no issues with grazing or grain when in heavy work becoming obese and laminitic within a month of stopping [work].”
Potential Complications
Once your horse has been diagnosed, it’s important to remain alert for possible complications. A common one is an uncontrolled appetite, which, if left unchecked, can lead to obesity.
Horses may also become more sensitive to common allergens, irritants, and vaccines. Hypertension and elevated triglycerides may develop, but by far the most significant complication is laminitis.
Regardless of potential problems, the bottom line is that there is significant hope for the future of any horse diagnosed with insulin resistance.
Related Conditions
The Equine Cushing’s and Insulin Resistance (ECIR) Group, Inc., was formed in 1999 to help share information and experiences among owners and professionals dealing with what is now known as pituitary pars intermedia dysfunction, or PPID. It was formerly and still colloquially called Cushing’s disease.
Equine metabolic syndrome (EMS), insulin resistance (IR), and PPID often have overlapping clinical signs that can make a diagnosis difficult. The ECIR Group works to help caregivers achieve that end.
With thousands of international members, the group’s discussion forum is arguably the largest field trial in the world for both PPID and EMS/IR. It provides the latest research, medication information, and dietary recommendations for horses with these conditions.
In 2013, the ECIR Group, an Arizona nonprofit corporation, was approved as a 501(c)(3) public charity. Tax-deductible contributions and grants support ongoing research, education, and awareness of PPID and EMS/IR. The group also hosts a NO Laminitis! Conference, five of which have been held since 2011.
For more information, visit their website at www.ecirhorse.org.
This article about insulin resistance in horses appeared in the March 2022 issue of Horse Illustrated magazine. Click here to subscribe!





