As horses age, one of the most common diseases that can develop is pituitary pars intermedia dysfunction (PPID). Long known as equine Cushing’s disease, the condition affects the endocrine system.
“The incidence of PPID increases with age,” says Kate Christie, DVM, a veterinarian with Rood & Riddle Equine Hospital in Lexington, Ky. “PPID is considered ‘uncommon’ in horses under 15 years of age. The prevalence increases to 20 percent of horses over the age of 15 years, and 30 percent of horses over the age of 30 years.” In rare cases, PPID has been diagnosed in much younger horses.

An example of a long, wavy haircoat that can be a sign of PPID. Photo by Christiane Slawik
One of the classic signs of PPID is delayed shedding or a long, wavy haircoat that doesn’t completely shed out. Other clinical signs include:
◆ Decreased athletic performance
◆ Change in attitude
◆ Lethargy
◆ Loss of topline muscling
◆ Tendon/ligament laxity
◆ Regional fat deposits (“cresty neck,” over tail head, above eyes)
◆ Laminitis
Out of Balance
As the name implies, PPID is directly tied to the pituitary gland, which is an endocrine gland located along the bottom of the hypothalamus in the horse’s brain. Because it controls hormone production, any dysfunction of this gland can cause problems.
“Age-related degeneration of the neurons that control hormone secretion from the pituitary gland leads to higher-than-normal levels of hormone production,” says Christie. “Increased ACTH (adrenocorticotropic hormone) production from the pituitary gland has many effects throughout the body.”
In simple terms, hormones become unbalanced because the pituitary gland is working overtime.
“One of the most important effects is the release of excessive amounts of cortisol (the stress hormone) from the adrenal glands,” she says. “These abnormal increases in hormone production are responsible for the main clinical signs of PPID.”
Diagnosis
If your horse shows clinical signs of PPID, there are two current methods of diagnosing the disease:
◆ Baseline ACTH (adrenocorticotropic hormone) test
◆ TRH (thyrotropin releasing hormone) stimulation test
Baseline ACTH is the best place to start in most horses when PPID is suspected. Because this hormone varies by season and reaches peak concentrations in the late fall/summer months, this test is also the preferred diagnostic for testing between June and December.
“If the baseline ACTH is normal but clinical suspicion is still high, a dynamic response test may be indicated,” explains Christie. “In the case of PPID, a thyrotropin releasing hormone (TRH) stimulation test is the most commonly used dynamic test.”
She adds that this test may be more helpful when identifying PPID earlier in the disease process. Because of seasonal variation in hormone production and the pituitary’s response to TRH, this test should only be run between January and June.
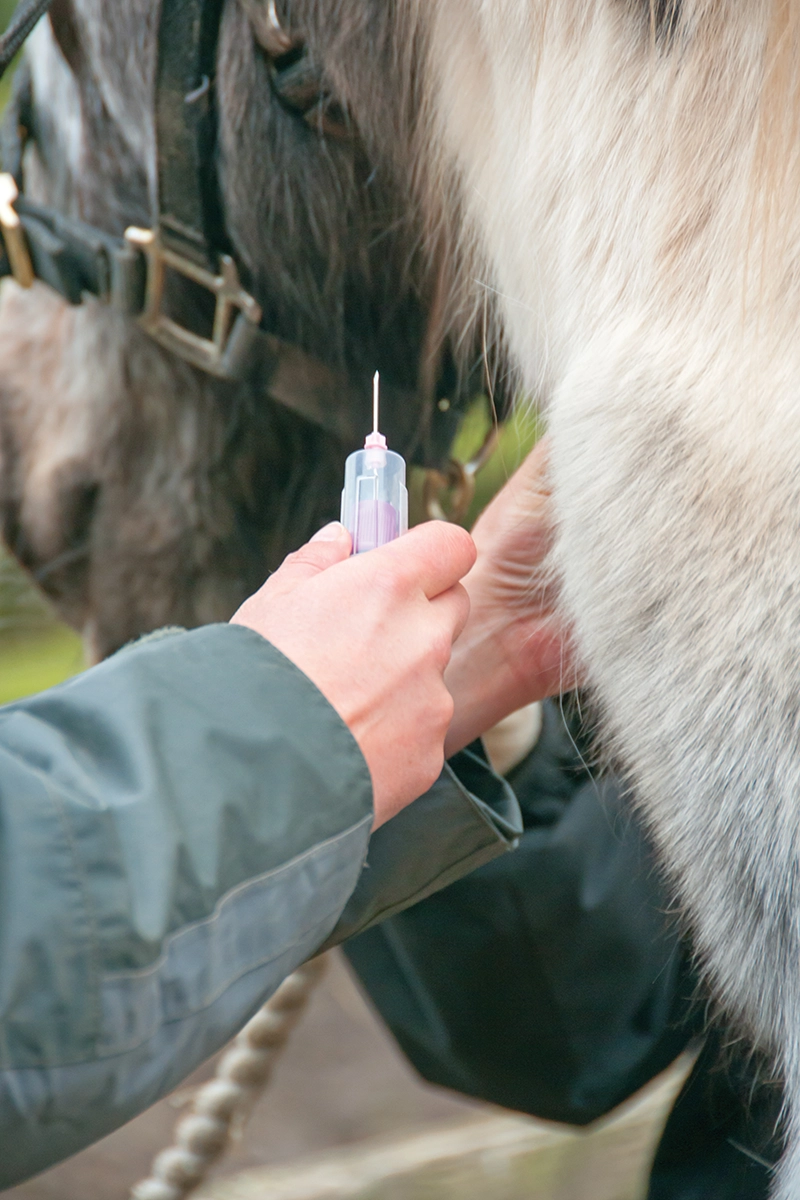
Baseline ACTH reaches peak concentrations in the late fall/summer months, so this test is the preferred diagnostic for PPID testing between June and December. Photo by Chelle129/Adobe Stock
Limiting Risk
Early diagnosis of PPID is important so that medical management can begin. If the disease is allowed to advance without treatment, worsening clinical signs can include:
◆ Sluggishness
◆ Exercise intolerance
◆ Infertility
◆ Excessive hair growth
◆ Topline muscle atrophy
◆ Rounded abdomen (“potbelly”)
◆ Weight loss
◆ Abnormal sweating (increased or decreased)
◆ Recurrent infections
◆ Bulging fat deposits above eyes (supraorbital fat)
◆ Laxity of tendons and suspensory ligaments
◆ Laminitis
Horses with PPID are often immuno-compromised. They tend to carry higher parasite burdens and be more prone to chronic infections, including rain rot, scratches, non-healing corneal ulcers, et cetera.
“Early diagnosis is important to prevent some of the more devastating complications of this disease,” Christie warns.
Laminitis Risk
Laminitis can develop in both early and advanced cases of PPID. The risk of laminitis is associated with increased insulin levels, which can be determined by testing.
“Approximately 30 percent of horses with PPID show signs of insulin dysregulation,” says Christie. “Insulin dysregulation is characterized by either a high resting insulin, a high postprandial (after feeding) insulin, tissue resistance to the actions of insulin at a cellular level, or any combination of these.”

Laminitis can develop in both early and advanced cases of PPID. The risk of laminitis is associated with increased insulin levels. Photo by Christiane Slawik
When insulin dysregulation is not controlled, the risk of developing laminitis is much higher.
Your veterinarian will likely suggest testing to determine your horse’s insulin status to assess the risk of laminitis and help decide the next steps, including any necessary changes in diet.
EMS May be a Factor
Some clinical signs of PPID can be confused with equine metabolic syndrome (EMS), and it’s possible for a horse to have both conditions. It’s important to realize that when a horse is diagnosed with both, the risk of laminitis is increased.
Having some degree of insulin dysregulation may indicate that a horse also has concurrent EMS. Christie points out that somewhere between 20 to 30 percent of horses with PPID also have insulin dysregulation that may be caused by underlying EMS, but a large subset of horses diagnosed with EMS do not have PPID.
Both PPID and EMS cause a disruption in metabolic function and increase a horse’s risk of hyperinsulinemia-associated laminitis. Although PPID and EMS can both be associated with insulin dysregulation, the pathophysiology of the two diseases is not the same.
Management, Not Cure
Although there isn’t a cure for PPID, medications are available for lifelong management, allowing horses to live comfortably.
The medication of choice for treating PPID is pergolide. An FDA-approved version of pergolide is available as Prascend (marketed by Boehringer Ingelheim).
When dealing with a medication that must be given for the rest of the horse’s life, owners often seek out better price options.
“Some pharmacies will compound this medication, and although it seems less expensive initially, the compounded versions are typically less [effective] than the FDA-approved product,” says Christie. “You[r horse] may require a higher dose of the compounded version to control clinical signs. Ultimately, the price advantage of compounded [medication] is negated by the decreased efficacy.”
She has found that some horses stop eating the medication in their feed, even when the pills are cleverly hidden in treats.
“While side effects are low, one major side effect is often decreased appetite, which can be really tough for older horses who already have body condition score concerns,” she says. “For these horses, splitting the dose into a twice-daily administration or decreasing the dose to a half or quarter of a tablet once a day for several weeks before increasing to one tablet may help.”
Christie has seen some cases where the horse cannot tolerate Prascend, or is poorly managed even on high doses of Prascend. This is typically only in late stages of the disease.
If clinical signs are not well controlled, or if your horse doesn’t tolerate Prascend, your veterinarian may add alternative medications, such as injectable cabergoline or cyproheptadine.
“The most important thing to understand is that medical management is just that—management,” says Christie. “Horses diagnosed with PPID require lifelong treatment and management, as well as close monitoring for worsening of clinical signs.”
Management Steps & Key Takeaways for Horses with PPID
In addition to daily medication, practical management is important when treating PPID.
Body clipping may be necessary for horses who no longer shed out completely.
“Depending on your horse’s insulin levels, specific dietary management may be recommended by your veterinarian to try
and control the risk of developing laminitis,” says Christie.
Your veterinarian may recommend switching to a diet that is low in non-structural carbohydrates (NSC). Concentrates aren’t the only concern. Hay and grass also contain sugar and starch, so managing PPID may include use of grazing muzzles or restricted turnout on grass.

Hay and grass contain sugar and starch, so managing PPID may include use of grazing muzzles or restricted pasture turnout. Photo by Jackienix/Adobe Stock
Certain supplements can also help manage insulin sensitivity.
Fecal testing has shown that horses with PPID have higher strongyle egg counts. Ask your veterinarian about recommendations for deworming protocol.
For horses showing any signs of laminitis, consistent farrier care is crucial.
“Work closely with your veterinarian and your farrier to monitor any changes in your horse’s overall or hoof health to prevent laminitis,” urges Christie.
Because PPID can be managed, it’s important to be aware of clinical signs of the disease. Have your horse tested promptly if signs develop.
This article about PPID in horses appeared in the March/April 2025 issue of Horse Illustrated magazine. Click here to subscribe!





