
The signs are obvious: A couple of scaly, crusty areas on your horse where the hair has fallen out. Your horse has some sort of skin disease, but what? And, more importantly, what should you do? Attempt to treat your horse yourself but risk a delay in getting the right kind of treatment for your horse? Summon the veterinarian to your farm, only to be told to administer a common, over-the-counter medicated shampoo?
Knowledge is Half the Battle
Effective treatment begins with appropriate treatment, and the foundation for appropriate treatment is recognizing the skin condition.
“Skin diseases are caused by infectious agents (bacteria, fungi, parasites, viruses), allergies (to insect bites, dietary factors, drugs, environment), abnormal reactions to sunlight, physical and chemical agents, hereditary factors, or they can be neoplastic [cancerous] in origin,” explains Sandy Sargent, DVM, resident in veterinary dermatology at the University of Tennessee.
Many of these disorders share the same appearance—various degrees of hair loss, itchiness, lesions that may or may not be painful to the touch, oozing sores or skin that is reddened, crusty, scaly, flaky, thickened or swollen. So while clinical signs and history are sometimes all that’s needed to identify some problems, other skin conditions require testing to diagnose. Consequently, the absence of an accurate diagnosis makes it trickier for the horse owner to supply a successful best-guess treatment.
Most skin diseases clear up quicker with early diagnosis and correct treatment.
“Diseases like pastern dermatitis (greasy heel, scratches) can be difficult to cure if the underlying cause is not diagnosed and treated early,” Sargent warns. “And while many diseases are self-limiting (they can and will heal on their own), inappropriate treatment can interfere with this healing process.”
That said, Sargent says that it’s usually OK for horse owners to try to treat mild cases of hair loss and crusty lesions with over-the-counter antibacterial and antifungal shampoos and/or sprays.
“Look for products containing chlorhexidine or Betadine,” she says. “Avoid products that do not list ingredients. Be sure to rinse the shampoo out well and dry the horse quickly, as a persistently damp coat can be a cause of skin problems. If the horse has a thick winter coat, spot-treat the affected areas instead.”
If the condition worsens soon after applying a topical product or doesn’t improve within seven to 10 days, stop the treatment and call your veterinarian. You should also seek veterinary advice if multiple horses, people and/or other contact animals are affected; if the lesions grow or spread rapidly, or if any tumors are found.

Skin Specifics
To help you better understand the most common (and not so common) skin problems that affect horses, here’s a closer look at causes and cures.
- Dermatophilosis (rain rot, rain scald, mud fever) is a bacterial infection aggravated by prolonged exposure to moisture coupled with injured skin. “Chronically infected animals are the primary source of infection,” Sargent explains. “Transmission can occur by flies, ticks, grooming equipment and tack. Once the disease has occurred within a barn or an individual horse, it is generally there to stay, just waiting for favorable weather conditions to reappear. In fact, any horse can be infected and once they have been, will often get it every year.”Look for: Lesions over the back and rump, although any area can be affected. “The lower layer of hair is firmly matted in small scabs which, when plucked may leave a characteristic ovoid [egg-shaped] bleeding surface,” Sargent says. “The undersurface of the scab is concave with the roots of the hair protruding and may have a covering of yellowish-orange pus. The affected areas are sore to touch, but are not itchy to the horse.”Treatment: Often resolves spontaneously after moving the horse to a dry environment. Also helpful is daily bathing with antimicrobial shampoos (chlorhexidine or povidone iodine) for the first week, then twice weekly until healed. Severe cases require oral or injectable antibiotics.
- Staphylococcus aureus is a highly resistant bacterial infection, reports Fairfield T. Bain, DVM, who practices at the Hagyard Equine Medical Institute in Lexington, Ky.Look for: Warm painful skin, focal crusts, most commonly in the pastern region, but similar lesions elsewhere on the skin can occur. “In some cases, the infection seems to rapidly involve deeper tissues,” Bain warns. “If allowed to become chronic, the underlying tissue can begin to scar and thicken.”
Treatment: “With the increasing resistance issues of certain bacteria, especially Staphylococcus, it is important to obtain a culture and sensitivity pattern to make sure that the correct antimicrobial agent is selected,” Bain emphasizes. - Dermatophytosis (ringworm) is caused by various fungi. “The organism invades the hairshaft, weakening it and causing it to break off,” Sargent says. “Predisposing factors include age (young and aged), poor nutrition and crowded conditions. The fungi can persist in the environment for up to one year and therefore are an important source for reinfection. Horse-to-horse transmission is common, especially in groups of young horses or in sick horses that are immunosuppressed. Spread of the spores via infected tack, blankets, bedding, trailers or fencing can occur. It is rare for healthy horses to get ringworm more than once as usually a horse develops immunity after being infected.”
Look for: Small hairless lesions that sometimes look like hives and scaly or crusty areas, typically located in the saddle, face and neck areas. Lesions may or may not be itchy or painful.Treatment: “Ringworm is usually self-limiting, with the horse getting better in one to three months without treatment,” Sargent states. “Exposure to sunshine is thought to be beneficial. To shorten the course of the disease, affected horses can be treated topically with a wide variety of antifungal treatments, such as chlorhexidine, miconazole, nystatin, terbinafine, et cetera. Widespread lesions are best treated with antifungal rinses or dips, such as lime sulfur or even diluted vinegar. Disinfecting the environment, tack and grooming equipment with diluted bleach or commercial antifungal premise sprays is extremely important.”
- Lice and mite parasitic infestations most commonly occur in late winter and early spring when the horse’s hair coat is at its longest.
Look for: Extreme itchiness. Additionally, horses troubled by lice often rub or bite at affected areas (usually the legs).Treatment for both problems: Includes topical insecticides, selenium sulfide shampoos, lime sulfur dips and oral dewormers, such as ivermectin. All in-contact horses and the environment must be treated. Treatment often needs to be repeated at least once, as new lice and mites can hatch from eggs (which are impervious to treatment).
- Culicoides hypersensitivity is an allergic response to gnat bites. “This very itchy disease is initially seen only in the warmer months,” Sargent reports. “As affected animals age, the disease generally becomes more severe and reactions can be seen year round.”
Look for: Peeling skin, crusts, scaling, hair loss and redness primarily involving the forehead, crest of neck, withers, shoulders, rump, ventral midline and the base of the tail.Treatment: “There is no cure, therefore, management is extremely important in providing comfort to these allergic horses,” Sargent says. “Since culicoides are primarily night feeders, keep the horse inside from dusk to dawn. Fly spray repellent is a must. In severely affected horses, prednisone is usually necessary to control the itchiness.”
- Squamous cell carcinoma is a malignant skin tumor of the outermost layer of the skin. It’s primarily found in light-colored skin, eyelid area, genital area and occasionally the mucous membranes.
Look for: Reddened, roughened or ulcerated skin.
Treatment: Removing or debulking the tumor, chemotherapeutic drugs, cryosurgery (destruction of unwanted tissue by freezing), anti-inflammatory therapy or radiation therapy. - Sarcoids are the most common skin tumors of the horse, Sargent says. “Thought to be viral in cause, sarcoids frequently occur in areas subject to trauma and may spread to other areas on the same horse or to other horses through biting, rubbing, fomites (inanimate objects such as tack, grooming tools, et cetera) or insects.”
Look for: Wart-like, proud flesh-like or flat plaque surfaces, usually on the ears, lips, neck and ventral abdomen or around the eyes.
Treatment: Surgical removal, topical therapies. - Equine ear papillomas are viral-induced skin tumors likely transmitted by black flies, Sargent reports. They occur in horses of all ages.
Look for: Warts in the ear.
Treatment: Topical products, although rarely effective. - Viral papillomatosis (warts) are also viral-induced tumors that occur in young horses less than 1 year of age.
Look for: Small warts on the muzzle and lips.
Treatment: “Spontaneous resolution usually within three months, although a vaccine made from the wart itself has been used and may speed resolution,” Sargent says. “Surgical excision or cryosurgery are effective if removal for cosmetic reasons is needed.”
- Melanoma is a common tumor in older horses and is seen more often in gray or white horses.
Look for: Round, nodular or ulcerated slow-growing lumps underneath the tail, perianal region; less commonly on the lips and base of the ears.
Treatment: Surgical excision unless tumors are numerous.
- Pemphigus foliaceous is a relatively common autoimmune skin disease that can become very severe and affect much of the body. “Because of the severe crusting it can be very painful,” says Bain. It usually affects horses age 5 years and older.
Look for: Painful crusty or blistering skin most commonly affecting areas on the head and lower extremities, although other areas can be involved. Lesions tend to develop in waves and coalesce to form larger and more diffuse areas of crusting.Treatment: “Often a lifelong process, involving the use of significant immune-suppressive medications (corticosteroids and other immune-suppressive drugs),” Bain states.
- Bullous pemphigoid-like disease is a blistering, autoimmune disorder occasionally seen in foals. “This condition results in blisters that progress to ulcers in the mouth, around the eyes and anus,” Bain explains. “This may be due to antibodies in the mare’s colostrum that react to certain components of the foal’s skin.”
Look for: Blisters around the mouth, eyes and anus. Affected foals often drool and do not nurse well.Treatment: Generally involves antibiotics and topical treatment of the oral ulcerations to aid in healing, sometimes supplemental feedings until the oral ulcerations heal.
- Allergic contact dermatitis occurs when irritating substances come into direct contact with the skin of hypersensitive horses. Irritants vary, but can include bedding, fly sprays, shampoos, liniments, et cetera.
Look for: Lesions occur in areas that come in contact with the offending substance and vary from mild redness, flaking and itching to severe hair loss, skin thickening, pain and occasionally skin sloughing.Treatment: Remove the causative substance and wash the skin with copious amounts of water. “In severe cases, topical or systemic anti-inflammatories and antibiotics may be required,” adds Sargent.
- Urticaria (hives) is a common, allergic response that can be caused by many things, including diet, insect bites and drugs (the most common cause).
Look for: The sudden appearance of hive-like lesions, which can occur anywhere on the bodybut typically on the face, neck, chest and upper legs, Sargent says. “They may or may not be itchy. Lesions typically last from a few hours to a few days.”
Treatment: Identifying and eliminating the causative agent. According to Sargent, “Severe urticaria reactions can be treated with antihistamines (hydroxyzine hydrochloride) and corticosteroids.”
- Photosensitization is an abnormal, inflammatory skin reaction to UV light that occurs in areas with white hair and pink skin. “A systemic disease, there are two forms of photosensitization,” Sargent explains. “A primary form associated with eating certain plants (St. John’s Wort, oats, clover, vetch, alfalfa, et cetera), and a secondary form that occurs with liver disease.
Look for: Skin that becomes swollen, red, cracked and oozing. In many instances there will be loss of skin. With secondary photosensitization, the horse will also be itchy.Treatment: “Primary photosensitization is treated by eliminating access to the offending plants and keeping the horse out of the sun,” Sargent says, noting that topical antibiotic/steroid ointments are also beneficial. “With secondary photosensitization, treatment is directed toward managing the liver problem.”
- Pastern dermatitis (greasy heel, scratches, mud fever, cracked heels) is a syndrome caused by a variety of diseases including bacterial infections, dermatophilosis, fungal diseases such as ringworm, chorioptic mange, irritant contact reactions, photosensitization, et cetera. Draft horses with a lot of feathering on their legs seem to be particularly susceptible.
Look for: Inflammation and foul-smelling crusts on the rear half of the pasterns and matted hair.Treatment: Treat the underlying cause; remove the horse from unsanitary, wet conditions; and minimize contact with irritating chemicals, plants, et cetera. Gently clip and clean the area, and apply shampoos, soaks, topical or systemic antibiotics and/or steroids per veterinary recommendation.

Risk Reducer
You can help reduce the risk of your horse developing skin problems by utilizing appropriate management practices. “Good insect control is very important, as insect bites and insect allergies are a common cause of itchy skin,” Sargent says.
Avoid excess bathing with shampoo, which can contribute to or cause skin disease. Limit your horse’s exposure to rain, provide shelter for outside horses, and groom regularly (but not excessively) with clean grooming equipment. Don’t share tack or grooming supplies with affected horses. “Frequently run your hands over your horse,” Bain says. “This can be one important way to find skin disease as you might feel a nodule or crust before it becomes visually obvious.”
Be wary about using home remedies recommended by other laypeople. “Some can be very irritating to the skin,” Sargent warns. “Products containing full strength iodine, alcohol, hydrogen peroxide, bleach, fungicides, turpentine, kerosene, motor oil, Listerine, et cetera. My rule of thumb is if I wouldn’t put it on my own skin/wound, I wouldn’t use it on my horse!”
Stay away from products that don’t list ingredients, and avoid using multiple products or switching from one product to the next from day to day; this makes it difficult to determine whether any one product is working or whether the products themselves are perpetuating or causing skin lesions. Only use products developed for horses—they are made to address equine pH levels.
Should your horse develop skin problems, don’t push the panic button. With mild cases, shampoo or spray with antibacterial and antifungal products, as described earlier, and monitor your horse’s condition. If you don’t see improvement within seven to 10 days, or your horse’s skin problems spread or worsen, summon your veterinarian.
Further Reading
Mud-Related Health Problems
Marcia King is an award-winning freelance writer.
This article originally appeared in the August 2005 issue of Horse Illustrated. Click here to subscribe.




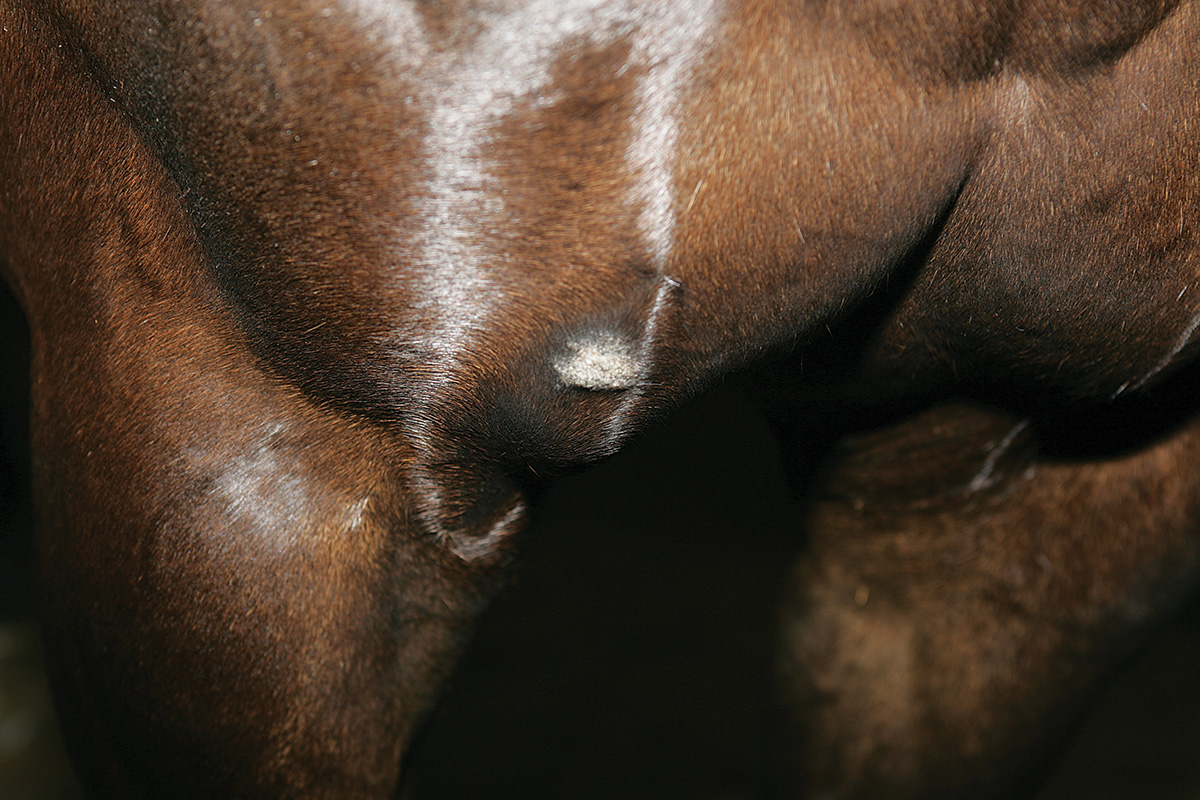

our quarter horse socrates has always seemed to have very sensitive skin, he gets rain rot easily as well as scratches. for the most part we have kept these under very good control. But recently he has developed hives once again in areas that have no contact with water, they don’t seem to be associated with any new drugs,supplements, insect bites and do not follow a pattern of contact dermatitis. Their history includes the formation of wheels/hives in a grouping that do not seem to itch or bother our horse they resolve by turning into a head with a small loss of hair as the scabs fall off. But not similiar to the rain rot pattern of hair loss, we have seen before. could you give us any suggestions as to what we are dealing with and how we might prevent it or treat it. Sincerely, Judith.
our quarter horse socrates has always seemed to have very sensitive skin, he gets rain rot easily as well as scratches. for the most part we have kept these under very good control. But recently he has developed hives once again in areas that have no contact with water, they don’t seem to be associated with any new drugs,supplements, insect bites and do not follow a pattern of contact dermatitis. Their history includes the formation of wheels/hives in a grouping that do not seem to itch or bother our horse they resolve by turning into a head with a small loss of hair as the scabs fall off. But not similiar to the rain rot pattern of hair loss, we have seen before. could you give us any suggestions as to what we are dealing with and how we might prevent it or treat it. Sincerely, Judith.
our quarter horse socrates has always seemed to have very sensitive skin, he gets rain rot easily as well as scratches. for the most part we have kept these under very good control. But recently he has developed hives once again in areas that have no contact with water, they don’t seem to be associated with any new drugs,supplements, insect bites and do not follow a pattern of contact dermatitis. Their history includes the formation of wheels/hives in a grouping that do not seem to itch or bother our horse they resolve by turning into a head with a small loss of hair as the scabs fall off. But not similiar to the rain rot pattern of hair loss, we have seen before. could you give us any suggestions as to what we are dealing with and how we might prevent it or treat it. Sincerely, Judith.
I found this article very helpful. I will now have a better idea of what I see and how to treat it or call the vet.
This page was VERY useful when I needed to find out what was wrong with my Arabian. It told me what I needed, if I needed a vet and how it should be treated! This also told me directly what had happened to my precious Arab. You guys are awesome, thanks so much!
wooooooof. alot to take in, but thanks for the article. very informative.
thanks this article was great help thanks
Hi, I had the vet out and he said our mare was allergic to flys. We put her own allergy shots for a year, but it has not helped. she is black, but now her face as white spots all around the sides. Is there anything I can do. She is covered haid to tail with fly sheet and hood, fly mask if she’ll leave it on and I even bought her fly boots, but she won’t leave them on. We have flys, but not that many.
This article was very useful!!! I had a hard time finding the treament for the diseases!! I also did a 4-H presentation and got almost all my info from this article!!! Thank you!!
Thank you. Very usefull information.
I have found two products that have almost completly cured my Icelandic horse of his severe case of sweet itch caused by the gnat, The first is the use of flygone 7000 and a horse cream from Iceland that will heal the soars within days and have hair going back in a week, it’s made by a lady in iceland and as far as I can tell from the bottle the ingrediants are all natural. I spent 8 years battling this and finally found this lotion thru an article that I found on the net. If anyone is interested in the lotion and how to get it please feel free to email me. I was hard to locate but works fantastic, not to expensive either. Also a fan on the horse and in from dusk to morning helps, but I keep my guy out 24/7 and he is doing very well for the second summer in a row.
For information on a lotion that you can get from Iceland for horses that will heal summer sweeth itch and most other types of irritations that horses get on their skine please email me, iceryder@comcast.net
My 7 year old Arabian/QH mare has bad crusts all summer mainly on legs and chest, she was almost eating her legs up. I stopped all chemicals on her, and finally found a lotion that seems really to work: Publix Brand Baby Lotion. It is in a white tube with the little blue 3wheeler on it. It keeps the skin smooth and heels the wounds like nothing I tried in the last 3 years. It is at least a try worth!
Good article.I have horses who have sweet itch all summer,and get rain rot in fall.I
use MTG mane tail grow solution with great results.It is a bit smelly,but the horses get such relief,and it seems to cure any skin problem.
The mare in the stall next to my mare has what I think is some form of rain rot(open stall barn). I live in Phoenix so its not caused from moisture. Her hair is greasy and you can pull it out in huge clumps. I think its caused from her owners NEVER bathing her. Well mow my mare is starting to lose hair on her rump. At first I thought it was from her going into heat, but it started spreading up her rump. The skin is not bleeding, but just going bald. When I try to scrub the area (thinking it was caused from her being dirty around there) or scratch at it the hair just falls out. Again we live in a vary hot dry place so i have no idea what could be causing it. Any suggestions short of calling a vet?
We have a saddle barn in a state park and we have had some problems with RAIN ROT. We have found that any kind of oil that we have used works well to kill the rain rot. Baby oil is one that is fairly inexpensive and seems to work well.
We have a saddle barn in a state park and we have had some problems with RAIN ROT. We have found that any kind of oil that we have used works well to kill the rain rot. Baby oil is one that is fairly inexpensive and seems to work well.
if your horse has rain rot or any sort of problem with greasy clumps of hair falling out one of the best things for it is pig oil it is widely available in any good farm shop and is completely safe for horses, my 2 horses had a problem with rain scald and this made it better within a matter of weeks.
I heard that tea tree oil helps rain rot. Has anyone had experience with this?
my two horses have these small scab like clumps in their hair and have for a while they have appered by their flanks and under the jaw when the curry occasionaly pulls one out they step away or flinch does anyone know what this is?
Always use caution when applying pure tea tree oil to any animal. It can be toxic if swallowed. Tea tree oil is commonly used in shampoos and is highly diluted and therefore should be safe in a shampoo, but once again, don’t use pure tea tree on any animal where they can get their mouth on it.
Hello, I have a 15 year old paint, with fist sized areas of what appears to be rubbed hair on each rear thigh, there are some scabs under the hair, but I can see no bugs, the hair that is left in the rubbed areas is bare to half an inch in length.
Hi,
I have a 4 year old gelding who has what seems to be hair loss on his chest and neck. But when you touch it hair is there. It is small circles all over his chest and neck. Does not bother him at all and feels normal to touch. I have 7 horses and he is the only one wiht this. My vet has never seen this wither. It is more cosmetic bu has to come form something. Any ideas? He is a red dun and spots look kinds black, but like I said haor is there just looks like it is missing. Thanks.
My 30 year old grey mare has a small lesion to the left of her tail near her anus on the ‘cheek’ It is weeping a black ink like substance, not blood, thin and watery. Daily bathing hasn’t helped. She doesn’t seem bothered by it. Could it be a parasite or a foreign body in there? Any ideas please. Mary.
I have a 8 yr old galding morgan quarter horse.
He has a sore inside his nose,one in each nostral.they are small but open.I put some triple anti biodic ointment on it.is it possible to get herpes in the nose.he’s in with a mare that has herpes warts.Vet said my horse is ok to be pastured with her.
so much information
Thank you! Still don’t know what it is but I feel much better after reading.
First of all, this is the best and most informative article I’ve ever read on this subject. However, I have a 12 yr old paint that has dry, scaly, dandruff, thinning of hair, patchy hair and quarter size areas where the hair is gone and the pink skin can be seen. He has been to 4 vets over the last few years that took all kinds of tests and biopsies, been on all the medications and nothing has worked. We live in dry California but right now it has gotten worse. He was on Prednisolone for a couple of months last year and he was looking better but it did not cure the condition. If you have any thoughts on this, I would love to hear them. Thanks!!
A Very informative article. We have been struggling to manage our pony for 4 years. Have had biopsy and using steroidal cream but its spread from top of face down her nose. She s hairless and very hot skin. Is indoors from sun every day. Seems to disappear in winter. VERY exasperated owner and less hopeful of finding cure.
Hi I find that using Equisan-H for disinfecting and sanitizing in all areas your horse sleeps and eats will help a great deal in reducing the cases of skin disease. Always remember to sanitize and disinfect things that your horse may come into contact with. Ex: Stalls, brushes, rub rags, blankets, tack etc.….Equisan-H cost less than $2.00 per bottle you should be able to find this product in your local tack shop the only Eco-friendly product that is ph balanced without harsh smell that is super easy to use. I just love Equisan-H disinfectant sensitize 😉
Prednisone weakens the immune system tremendously. I have a 12yr old WB mare that came from NJ to FL and couldn’t handle the bugs. She was scabbing up and ripping her hair off. The only thing that worked was a combination of herbs that I researched online. The #1 herb that works is spirulina powder the other ingredients would depend on your issues.
I also buy minced garlic in a jar and put it in there feed, very good antifungal.
Thank you so much horse illustrated for sharing this information. It’s been very helpful for me to have a better understanding to care for my horses skin conditions.